Trump's hydroxychloroquine use underscores line between drug's promise and 'happy talk'
President Donald Trump surprising disclosure on Monday that he was using hydroxychloroquine, an anti-malarial drug commonly used by lupus and rheumatoid arthritis patients, has amplified an already fierce debate over its use for coronavirus patients.
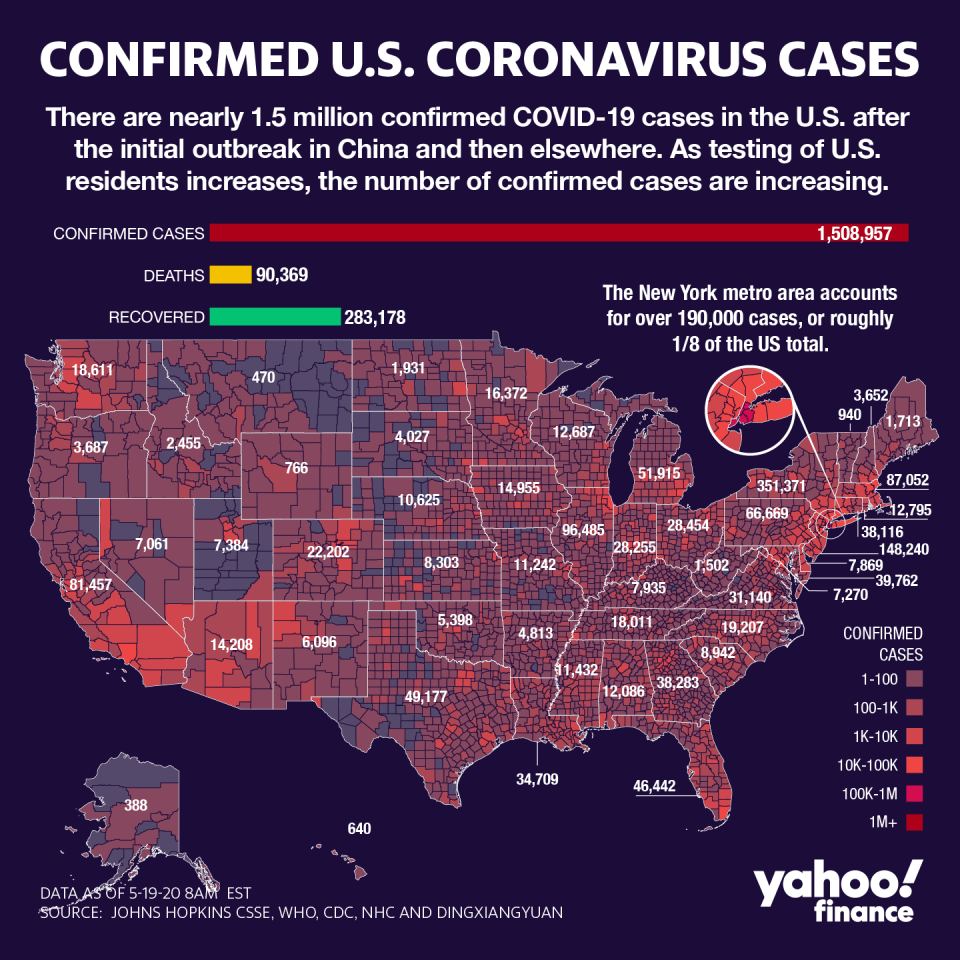
Trump, who said he asked to be and was then prescribed the drug by the White House physician, has spent weeks touting the drug as a potential “game-changer” in the fight against COVID-19, which has sickened around 1.5 million Americans with the death rate creeping toward 100,000.
Yet the president’s use of hydroxychloroquine as a preventative measure — along with its already flagged risks — triggered heated discussions about the wisdom of the decision.
Weeks after issuing an emergency use authorization for both hydroxychloroquine and a similar drug called chloroquine, the U.S. Food and Drug Administration (FDA) warned they were not “safe and effective” when used on COVID-19 patients.
Still, Trump insisted on Monday that “a lot of good things have come out about the hydroxy(chloroquine). You’d be surprised at how many people are taking it, especially the frontline workers before you catch (the virus).”
Trump initially sparked a furor when he first floated hydroxychloroquine as a potential treatment in the COVID-19 fight. He doubled down on its potential Monday, repeating his previous conviction that it is not a harmful drug, used for off-label uses, and has been around for 40 years. In recent weeks, several health experts have warned about its potential harm.
The president, meanwhile, said he has been taking it for a couple of weeks. “Frontline workers take it. A lot of doctors take it.”
‘Happy talk’
But according to Henry Miller, founding director of the FDA's Office of Biotechnology and a Senior Fellow at the Pacific Research Institute, Trump’s public advocacy of the treatment — and the FDA’s initial decision to authorize an emergency use order — is giving the debate a needlessly political veneer.
“It’s an example of an FDA action that in a sense was unnecessary...probably politically motivated,” Miller told Yahoo Finance in a recent interview. He also blasted the FDA’s emergency use authorization as unnecessary, because the drug is already approved for off-label uses like lupus and rheumatoid arthritis.
Miller charged that much of the discussion surrounding coronavirus treatments has been tainted by “politically motivated happy talk” that is affecting how officials should interpret the data.
“I’m a Republican, but I resent happy talk, I resent misrepresentation and I resent lies,” Miller added.
The agency’s guidance issued on Thursday stopped short of banning its use altogether. Instead, the FDA recommended consumers do not use it independently, and said health professionals should use their judgement when prescribing it for a coronavirus patient.
Trump’s effusiveness was stoked by a couple of inconclusive early studies, one of which was conducted in France. Yet the FDA’s decision amplified the findings of other studies, including a preliminary report from the Department of Veterans Affairs, that suggest the drug may pose more of a risk when used to treat COVID-19 patients.
“It’s upsetting because there is only anecdotal data, except for the extremely questionable French studies and there are real holes in that,” Miller said, adding France’s study has “puzzling flaws.”
While there haven’t been any reported deaths linked to the French study, there are lingering concerns about toxicity and what the tradeoff of benefits and risks are.
A drug with anecdotal promise, and risks
Despite the debate at the federal level, hydroxychloroquine has some prominent advocates involved in the fight against the pandemic.
Recently, Novartis (NVS) CEO Vas Narasimhan told a German newspaper that pre-clinical data in animals and initial clinical studies show the drug actually kills the virus. The drug is produced by Novartis’ Sandoz division, and Bayer (BAYRY) produces chloroquine— both of which have donated millions of doses to the national stockpile. Teva (TEVA) and Mylan (MYL) also make hydroxychloroquine.
Meanwhile, New York state has been allowing the use of hydroxychloroquine in hospitals, anticipating better data as the drug is used in empirical settings. Gov. Andrew Cuomo has cited its anecdotal effectiveness, but said last month that initial studies show its results to be neutral at best.
Dr. Anthony Fauci, the leading White House coronavirus task force member, has previously expressed more caution about using hydroxychloroquine in COVID-19 treatment protocols, saying there has only been “anecdotal evidence,” about its effectiveness.
Dr. Ezekiel Emanuel, who served as special advisor for health policy to the director of the White House Office of Management and Budget during the Obama administration echoed those remarks in a recent talk with Yahoo Finance in which he said “we need to rely on data.”
As the public debate ramps up, its sparked increased demand for hydroxychloroquine — something that’s prompted other states — such as Ohio, Texas, and Nevada — to protect access for patients who need the drug for off-label uses. Reports of doctors ordering it for themselves, friends and family, have resulted in supply shortages.
Miller, however, hopes the FDA’s rush to validate hydroxychloroquine doesn’t spill over into approvals of other COVID-19 treatments and vaccines in the pipeline.
“I hope that [FDA Commissioner Steven Hahn]... won’t be rushed unnecessarily or inappropriately for insufficient evidence of data,” he said, citing vaccines as a particular worry.
Public officials have cited a timeline of 12 to 18 months for a potential coronavirus cure. However, Miller blasted that as “politically motivated happy talk” and “off by a factor of two, at least.” Fauci is among those who have floated that optimistic time frame, given the urgency of the crisis.
Yet Miller stated that “Fauci has qualified it in a clever way. He says a vaccine that you make and start testing in a year is not a vaccine that is deployable. You can have a candidate, but can’t complete all required testing in a year.”
Anjalee Khemlani is a reporter at Yahoo Finance. Follow her on Twitter: @AnjKhem
Read the latest financial and business news from Yahoo Finance
Follow Yahoo Finance on Twitter, Facebook, Instagram, Flipboard, SmartNews, LinkedIn, YouTube, and reddit.

 money
money 
